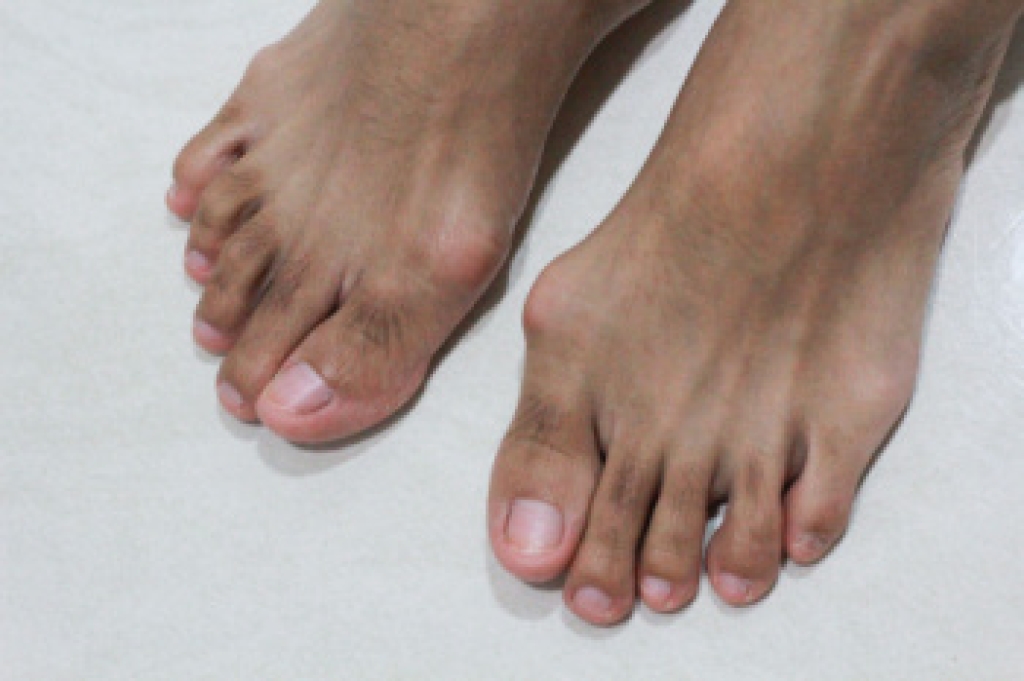
Haglund’s deformity is a bony bump that forms on the back of the heel near where the Achilles tendon attaches. This prominence can rub against shoes, especially those with stiff backs, causing irritation, redness, and pain. Over time, it may also lead to inflammation in nearby tissues, making walking uncomfortable. Other conditions can feel very similar and are sometimes confused with this issue. These include irritation of the Achilles tendon, inflammation of the fluid-filled sac near the heel, or general overuse injuries. Because symptoms overlap, proper evaluation is important to confirm the cause of pain. Treatment often begins with simple changes like wearing softer shoes, using padding, adding heel lifts, and doing stretching exercises. If discomfort continues despite these efforts, a minor surgical procedure to remove the extra bone may be considered. If heel pain is limiting your daily activities, it is suggested that you schedule a visit with a podiatrist for a proper diagnosis and appropriate treatment.
Many people suffer from bouts of heel pain. For more information, contact Sharmila Das-Wattley, DPM of Home Wound Healing. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions, please feel free to contact our office located in Florida . We offer the newest diagnostic and treatment technologies for all your foot care needs.